por Kiko Ramos | Mar 12, 2025 | Equipment analysis
The interventional radiology (IR) is a specialized branch of the radiology area that combines techniques of diagnostic imaging with minimally invasive therapeutic procedures to diagnose and treat different diseases. In contrast to traditional surgical procedures, which require large incisions and long recovery times, interventional radiology allows for treat diseases without the need for open surgery. In this way, it stands out as an innovative discipline that reduces risks, recovery time and postoperative complications.
In the last decades, interventional radiology has experienced a great growth with the development of new technological advances both in imaging techniques and in medical equipment for the diagnosis and treatment of patients. interventional radiology. In the following article, we analyze what it consists of, its different types, as well as its main advantages and disadvantages.
What is interventional radiology?
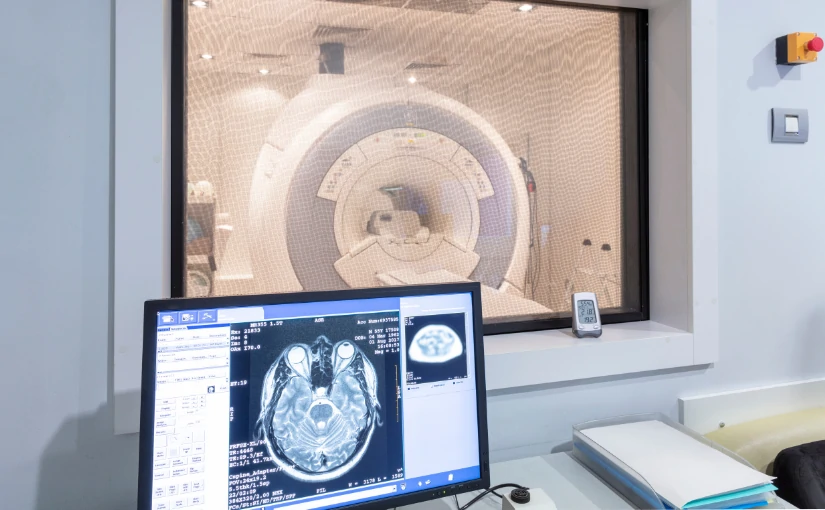
Interventional radiology uses a series of diagnostic imaging technologies to guide therapeutic procedures with a high precision. The main modalities used are the following X-raysthe ultrasoundsthe computed tomography (CT) scans and the magnetic resonance imaging (MRI).
These techniques offer detailed information on the patient's anatomy and physiology in real timeThis allows medical professionals to visualize specific areas of anatomical structures and access them by making small incisions. To do so, they use specialized instruments such as catheters and needles. The use of high quality images and live viewing capability during procedures not only facilitates device placement, but also plays a key role in minimizing the risks associated with the procedure and reducing damage to healthy tissues.
IR is a medical discipline that is used for the treatment of treatment of various medical specialtiesThe company's main areas of expertise include oncology, cardiology, neurology, vascular radiology and musculoskeletal medicine. In turn, it has the capacity to offer less invasive procedures for patients who have certain risks in conventional surgery, such as the elderly, as well as patients with advanced pathologies or with a high surgical risk.
Interventional radiology procedures are performed under the following conditions local anesthesia, patients are awake during the procedure. Therefore, the risks that may arise from the application of general anesthesia are reduced. Another aspect to highlight is that most procedures are performed on an outpatient basis. In this way, patients can return home on the same day of surgery, reducing hospital costs and increasing the efficiency of the healthcare system.
The multiple advances in technology offer a great projection in interventional radiology. The integration of artificial intelligence in medicine and robotics has a special relevance in this discipline, which will increase precision and efficiency in the treatment of many diseases.
Types of interventional radiology
Medical technology continues to advance and interventional radiology plays a fundamental role in modern medicine. It is now used in different medical specialties and covers a wide range of therapeutic procedures. The main types of interventional radiology include vascular, oncology, musculoskeletal, gastrointestinal, urological, thoracic and gynecological, which we discuss below:

Guided image diagnosis
One of the main functions of interventional radiology is the diagnosis of diseases through image-guided procedures. In many cases, it is necessary to take tissue samples or drain fluids accumulated in the body to obtain an accurate diagnosis. Through the use of imaging techniques, these procedures can be carried out with a millimetric precision and without the need for invasive surgery.
Main diagnostic procedures
- Image-guided biopsiesBiopsies: Fine needles are used to remove tissue samples from organs such as the liver, lungs, thyroid or prostate. These biopsies make it possible to detect diseases such as cancer in its early stages.
- Percutaneous drainageWhen there is fluid accumulation due to infection or inflammation, catheters are placed to remove it without the need for major surgery.
- Puncture and aspiration of cysts or massesUsing a needle guided by ultrasound or tomography, physicians can remove cysts or reduce pressure in areas with fluid accumulation.
2. Vascular and endovascular treatment
The diseases of the circulatory systemsuch as arteriosclerosis, aneurysms and varicose veins can be effectively treated with interventional radiology techniques. In these cases, physicians use catheters and guidewires for accessing blood vessels and perform procedures that improve circulation or prevent serious complications. These treatments offer a less invasive alternative to conventional surgery, reducing hospitalization times and improving patients' quality of life.
Main treatments
- Angioplasty and stentingIn patients with blocked arteries, a balloon is introduced through a catheter to widen the blood vessel. Subsequently, a stent, a small metal device that keeps the artery open and prevents future blockages, is placed.
- Aneurysm embolizationWhen aneurysms, dangerous dilatations of the arteries, arise, micro-spirals or embolizing materials can be introduced to reduce the risk of rupture.
- Treatment of varicose veins and vascular malformationsSclerotherapy techniques are used to close abnormal veins and improve circulation, eliminating aesthetic discomfort and associated circulatory problems.
Clinical applications
- Peripheral arterial disease.
- Cerebral and arterial aneurysms.
- Stroke, cerebrovascular accident.
- Varicose veins and venous malformations.
3. Interventional Oncology
In the field of oncology, interventional radiology has opened up new possibilities for the treatment of cancer. canceras it allows the localized destruction of tumorsThe impact on healthy tissues and its side effects are reduced. Therefore, interventional oncology represents an important effective and less aggressive alternative to surgery.
Procedures in interventional oncology
- Percutaneous tumor ablationRadiofrequency, microwave or cryotherapy techniques are used to destroy tumors in the liver, kidney, lung and other organs without the need for open surgery.
- Chemoembolization and radioembolizationChemotherapeutic drugs or radioactive particles are administered directly into the blood vessels that feed the tumor, reducing its size and preventing its growth.
- Placement of catheters and central venous accesses.In patients requiring prolonged chemotherapy treatments, venous ports are inserted to administer the drugs more comfortably and safely.
Clinical applications
- Liver, lung and kidney cancer.
- Bone and soft tissue tumors.
- Palliative treatment in oncology.
4. Traumatology and pain management
Interventional radiology procedures are also essential for the management of chronic pain and the treatment of musculoskeletal injuries. These procedures improve the quality of life for patients by reduce pain and restore joint function without the need to resort to open surgery.
Most common interventions
- Joint infiltrations and nerve blocksAnesthetic and anti-inflammatory drugs are injected into joints such as the knee, hip or spine to relieve pain caused by arthritis or other conditions.
- Cementoplasty (vertebroplasty and kyphoplasty)In this type of procedure, a bone cement is injected into fractured or osteoporosis-damaged vertebrae to reduce pain and improve spinal stability.
- Aspiration of calcifications and drainage of articular cystsCalcium deposits in tendons or fluid accumulated in joints are eliminated, improving the patient's mobility and reducing pain.
Clinical applications:
- Osteoporosis with vertebral fractures.
- Herniated discs and chronic low back pain.
- Rheumatoid arthritis and osteoarthritis.
5. Gastroenterology and urology
IR can be used to treat diseases of the digestive and urinary tract.
- Placement of esophageal and biliary prosthesisStents are inserted in the esophagus, bile ducts or intestines to allow the passage of food or liquids in cases of obstructions caused by tumors.
- Percutaneous nephrostomyDrainage: A drainage tube is inserted into the kidney to decompress urinary obstruction in patients with kidney stones or tumors.
- Treatment of gastrointestinal bleedingEmbolization is used to stop bleeding from gastric ulcers or esophageal varices, avoiding emergency surgery.
Clinical applications in gastroenterology
- Esophageal, liver and pancreatic cancer.
- Hepatic cirrhosis with portal hypertension.
- Biliary obstructions and intestinal strictures.
Clinical applications in urology
- Urinary obstruction due to tumors or kidney stones.
- Varicocele and fertility problems.
- Benign prostatic hyperplasia.
6. Pulmonary and thoracic interventional radiology.
This specialty allows the diagnosis and treatment of thoracic diseases without the need for invasive surgical procedures.
Main procedures
- CT-guided lung biopsyLung tissue sampling for cancer diagnosis.
- Pleural drainage and pleurodesisElimination of fluid in the pleural space in cases of pleural effusion.
- Embolization of pulmonary arteriovenous malformationsClosure of abnormal blood vessels in the lungs.
Clinical applications
- Lung cancer and pleural diseases.
- Recurrent pneumothorax.
- Pulmonary vascular malformations.
7. Gynecology and obstetrics
In this medical specialty, the following treatments can be performed gynecological pathologies and pregnancy complications with image-guided procedures.
Main procedures
- Uterine fibroid embolizationNon-surgical procedure that reduces the size of fibroids without removing the uterus.
- Treatment of postpartum hemorrhageUterine arteries are occluded to stop severe bleeding after delivery.
- Pelvic abscess drainageGynecological infections elimination with percutaneous catheters.
Clinical applications
- Uterine fibroids and abnormal bleeding.
- Severe postpartum hemorrhage.
- Pelvic abscesses due to infections.
Meet our 4D Medical equipment
Advantages of interventional radiology
Interventional radiology offers many advantages and has transformed the treatment of many diseases, offering safer, less invasive procedures with shorter recovery times.
Minimally invasive procedures: Less risk and greater precision
One of the major advantages of interventional radiology is that it allows treatments to be performed without the need for open surgery. Instead of making large incisions, it uses small punctures in the skin through which catheters, microneedles and specialized devices are introduced.
This results in less damage to surrounding tissuesthere is a reduced risk of postoperative infections and you get a reduction of bleeding and scar formationimproving the patient's recovery.
Shorter hospital stay and faster recovery time
Interventional radiology procedures, being less aggressive to the body, allow the patient to recover in less time compared to conventional surgery. Many of the procedures are ambulatoryThe patient returns home after the procedure and is then hospital stay is reduced.
Another aspect to highlight is that the simpler and less invasive interventions. In this way, the decreases the consumption of painkillers since postoperative pain is less. At the same time, the patient can return to his or her daily activities and work in a shorter time, since the recovery times are shorter.
Less need for general anesthesia
Unlike traditional surgeries, which usually require general anesthesia, interventional radiology procedures are performed with local anesthesia and light sedation. This minimizes anesthetic risksespecially in patients with chronic diseases or advanced age. In addition to reducing the risk of complications, interventional radiology offers safer procedures for patients with cardiac or respiratory problems.
Highly accurate and efficient diagnosis and treatment
Interventional radiology uses real-time imaging to guide the placement of needles, catheters and other medical devices with extreme precision. The use of techniques such as fluoroscopy, ultrasound, computed tomography or magnetic resonance imaging offers different benefits:
- Helps reduce the margin of error in complex procedures.
- Increased success rate of oncology and vascular treatments.
- Reduces collateral damage in adjacent structures.
Alternative treatment for patients who are not surgical candidates
For many patients with advanced disease or high surgical risks, interventional radiology is the only viable treatment option. It is a alternative for people suffering from advanced diseaseshave severe comorbidities or for those who reject invasive surgical procedures.
Covers multiple medical specialties
Interventional radiology is not limited to a single medical specialty, but is also encompasses several areas. Therefore, it provides a versatile treatment for treating diseases in different organs and systems, since it its approach is multidisciplinary. In addition, it is a discipline that is constantly evolving, thus allowing the application of new applications and technological improvements.
Lower cost compared to traditional surgeries
Although some interventional radiology procedures may involve more expensive medical equipment, their total cost is lower than that of conventional surgery. Among the main factors that reduce its costs, we can highlight the following aspects:
- Reduced consumption of medical resources and hospitalization time.
- Medication is reduced administered to patients.
- Faster recovery.
Disadvantages of interventional radiology
Despite its many benefits, interventional radiology is not without its limitations and challenges. Although it represents a less invasive alternative to traditional surgery, there are factors that may limit its application or affect patient safety.
Limited availability and restricted access
One of the main challenges in interventional radiology is that not all hospitals and clinics have the necessary technology and trained specialists. to perform these procedures.
In rural areas or countries with fewer resources, patients may not have access to advanced imaging equipment or interventional radiologists, limiting the possibility of receiving these treatments. In these cases, patients will have to travel long distances to receive care, so many of them will have to opt for more invasive surgeries due to the unavailability of interventional radiology.
Another disadvantage is that not all health systems finance these procedures. and this may generate economic barriers that hinder access to this medical discipline.
Not all procedures are equally effective in the treatment of the disease.
Although interventional radiology offers effective solutions for many diseases, some procedures only control symptoms or slow disease progression, but do not completely eliminate the disease. Therefore, IR emerges as a temporary solution until the patient is able to undergo definitive treatment. On other occasions, some treatments must be repeated several times to increase its effectiveness.
Use of ionizing radiation in some procedures
Many interventional radiology procedures, especially those that utilize X-ray machines and fluoroscopy, expose the patient to ionizing radiation. Although the doses are usually low, repeated exposure may increase the risk to the patient.
What impact can it have on the patient? On the one hand, cumulative exposure over the years. could increase the risk of adverse effectsespecially in repeated procedures. In turn, in young patients or pregnant women, the risk-benefit ratio should be evaluated with caution.
Possible adverse effects and complications
Although interventional radiology is generally safer than surgery, it is not without risks and complications. As these are minimally invasive procedures, there is a possibility of adverse effects in certain patients:
- Hemorrhage at the puncture siteMay occur in procedures that require the insertion of catheters in arteries or veins.
- Allergic reactions to contrast mediumIn studies such as angiography and cholangiography, some patients may present severe allergic reactions to iodinated contrast material.
- Infection at the puncture siteAlthough less frequent than in conventional surgeries, there is still a risk of infection.
- Device migrationIn rare cases, a stent or embolization coil may dislodge and cause unwanted obstructions.
Recent discipline and limited availability of professionals
The success of interventional radiology depends largely on the skill and experience of the interventional radiologist. In contrast to traditional surgery, where surgeons have extensive experience, IR is a relatively new specialtyand, therefore, the availability of highly trained professionals is still limited.
Conclusion
Interventional radiology is a recent medical discipline that offers high precision, reducing the application of invasive treatments and open surgery. In recent years, it has had a great impact on modern medicine, improving the quality of life of patients and reducing postoperative complications, hospitalization times and health care costs.
Do you need more information about medical equipment? Contact us and from the 4D Médica team we will help you find the equipment that best suits the different needs of your clinic or medical center.
Contact 4D
Bibliography
Dalda Navarro, J. Á., Navarro Martín, M. T., Negre Ferrer, E., Negre Ferrer, C., Navarro Martín, A. B., & Dalda Navarro, V. (2024).
Interventional radiology: minimally invasive treatments under image guidance. Health Research Journal, 5(6). Retrieved from
https://dialnet.unirioja.es/servlet/articulo?codigo=9693488?
Lonjedo, E. (2019). Interventional radiology: as far as the image takes you. Annals (Reial Acadèmia de Medicina de la Comunitat Valenciana), (20). Retrieved from https://dialnet.unirioja.es/servlet/articulo?codigo=7710219
Kiko Ramos
CEO of 4D Médica. Expert in marketing and distribution of medical equipment.


por Luis Daniel Fernádez | Mar 10, 2025 | Equipment analysis
Ultrasound is a noninvasive medical technique that uses ultrasound to obtain real-time images of the inside of the body. The medical equipment used to perform an ultrasound scan is the ultrasound scannerwhich incorporates a device called a transducer. The ultrasound transducers are the main component of this medical equipment in the area of diagnostic imaging. They have the function of emitting high-frequency sound waves, which make it possible to observe the functioning and movements of the body's internal tissues and organs. Subsequently, they are responsible for generating the medical images that are displayed on the screen or monitor of the medical equipment, which are called sonograms.
The quality and usefulness of an ultrasound scan depend to a large extent on the transducer used. Therefore, in the following article, we discuss the operation of this device and provide a detailed guide to the different types of ultrasound transducers that exist. Do you want to know what their main advantages, functions and differences are? We will analyze them below!
Ultrasound transducers: Concept and operation
The transducer, also called ultrasound probeis the ultrasound component which converts electrical energy into sound waves, known as ultrasound. Its operation is based on the piezoelectric effect, a phenomenon in which certain crystals present in the transducer generate vibrations when receiving electric current, producing sound waves. In this way, the transducer or probe acts as a transmitter and receiver of
ultrasound.
When these waves penetrate the body and hit different structures and tissues, they return to the transducer in the form of echoes. Ultrasound scanners process this information and convert the captured ultrasounds into medical images that can be displayed on the equipment's screen. They are called sonograms and allow the following to be obtained visualize the functioning of the different tissues and organs in real time.
Use of transducers in ultrasound scanning
In the realization of a ultrasoundThe transducer plays a key role. The use of this device works as follows:
- Selection of the appropriate transducerThere are different types of transducers or ultrasound probes, so depending on the anatomical area to be evaluated, the physician or technician must select a specific transducer.
- Ultrasound gel applicationDuring an ultrasound scan, the transducer is coated with a conductive gel that slides over the patient's skin in the specific area to be analyzed. This gel eliminates the air between the skin and the transducer, which facilitates the transmission of the ultrasound waves and improves the quality of the images.
- Exploration of the area of interestThe transducer can be slid over the skin or inserted into a cavity in the case of transvaginal or transrectal ultrasound. While moving, the ultrasound scanner displays real-time images of the examined area on the screen.
- Parameter settingThe operator can modify certain parameters to improve image quality according to the depth and type of tissue to be analyzed. These include frequency, focus and gain.
- Image capture and interpretationSubsequently, the images generated are recorded for analysis and diagnosis, which creates an ultrasound scan that allows evaluation of the state of the organs and tissues.
Types of ultrasound transducers
Not all transducers perform the same function. Depending on the anatomical area to be analyzed, different resolutions and penetration depths are required. Therefore, a key aspect to increase diagnostic accuracy is to select the right transducers. transducers for ultrasound scanners adequate. To this end, it is important to to know the different options and models. Below, we provide a complete guide explaining the main types of transducers used in ultrasound along with their characteristics, advantages and clinical applications.

Linear transducers
Linear transducers are characterized by their rectangular shape and the emission of ultrasonic waves in parallel lines. They offer high resolution, but have lower penetration. They are mainly used for superficial studies in physiotherapy, podiatry and dermatology.
Advantages
- High image resolutionThis allows observation of fine anatomical details.
- Ideal for surface structuresThe frequency range is between 5 and 15 MHz.
- Excellent for vascular and musculoskeletal studies.
Clinical applications
- Vascular ultrasoundEvaluation of arteries and veins.
- Soft tissue ultrasoundThyroid, breast, muscle and joint examinations.
- Dermatological ultrasoundEvaluation of the skin and superficial structures.
Convex or curvilinear transducers
These transducers have a curved shape that allows a larger field of view at intermediate and large depths. They generate sector or fan-shaped images. They have a greater penetration compared to the linear transducer. They are used for abdominal and gynecological studies.
Advantages
- Increased penetration than the linear transducer, includes frequencies between 2 and 6 MHz.
- Suitable for abdominal and pelvic studies.
- Has a wide image coverageIt is therefore very useful in large organ scans.
Clinical applications
- Abdominal ultrasoundEvaluation of the liver, kidneys, gallbladder and pancreas.
- Obstetric ultrasoundPregnancy monitoring and fetal assessment.
- Pelvic ultrasoundExploration and evaluation of the reproductive organs.
- Studies in pediatrics and general medicine.
Sector or Phased Array Transducers
Sector transducers, also referred to as sector transducers, are phased arrayemit waves from a small spot. They emit waves in a narrow aperture scanning pattern and generate triangular or fan-shaped images. They have a high penetration, but have a lower resolution than linear transducers.
Advantages
- Allows scanning of deep structures without the need for extensive skin contact.
- Has a low frequency between 2 and 4 MHz, which guarantees excellent penetration.
- It is suitable for studies in confined spaces such as the thorax.
Clinical applications
- EchocardiographyEvaluation of the heart and large blood vessels.
- Pulmonary ultrasoundPulmonary parenchymal examination, diagnosis of thoracic pathologies and studies in intensive care.
- Emergency ultrasoundIt is used in FAST (Focused Assessment with Sonography for Trauma) studies in the area of trauma.
Endocavitary transducers (endovaginal and endorectal)
These transducers are designed to be inserted into body cavities and provide detailed, high-resolution images of internal organs at close range. This type of ultrasound probe is used in gynecology, obstetrics and urology specialties.
Advantages
- High image resolution due to its proximity to the organ to be examined.
- The frequency offered is intermediate-highThe resolution is between 5 and 9 MHz, thus offering a balance between resolution and penetration.
- Facilitates the detection of gynecological and prostate pathologies.
Clinical applications
- Transvaginal ultrasoundEvaluation of the uterus, ovaries and early pregnancy.
- Transrectal ultrasoundDiagnosis of prostate and rectal pathologies.
Microconvex transducers
This type of transducer is similar in design to convex transducers, but has a smaller surface area. Therefore, it is characterized by providing greater maneuverability in areas that are difficult to access. Among its different applications, microconvex transducers are used to perform examinations in pediatric patients, neonates and in the veterinary area.
Advantages
- Increased maneuverability in small anatomical areas.
- Intermediate frequency between 5 and 8 MHz, providing a balance between depth and resolution.
- It is the right choice for studies in patients difficult to explore with conventional transducers.
Clinical applications
- Pediatric and neonatal ultrasoundBrain and abdominal evaluation in neonates.
- Veterinary ultrasoundFor animal examinations.
- Studies in anesthesiology and intensive careIt is used as a guide for procedures such as catheter placement and punctures.
Volumetric transducers
These transducers generate three-dimensional images in real time using advanced technology with multiple piezoelectric crystals. They are used for 3D and 4D digital reconstruction to visualize anatomical volumes.
Advantages
- Detailed and volumetric images of anatomical structures.
- Allows evaluation of fetal morphology with greater precision.
- Enables navigation in advanced diagnostic studies.
Clinical applications
- Obstetric ultrasound in 3D and 4DDetailed evaluation of the fetus and detection of malformations and anomalies.
- Advanced gynecologic ultrasoundAccurate diagnosis of uterine and ovarian abnormalities.
- 4D EchocardiographyCardiac studies that allow the visualization of the heart in real time with high precision.
Special ultrasound transducers
In addition to conventional transducers, there are transducers designed for specific applications:
- Doppler transducersThey allow to evaluate blood flow in real time.
- Laparoscopic transducersMinimally invasive surgical procedures: They are used in minimally invasive surgical procedures.
- Array transducers or Matrix ArrayCapture multiple image planes simultaneously for more accurate reconstructions.
Meet our 4D Medical Ultrasound Transducers
Guide to choosing the right ultrasound transducer type
Selecting the right ultrasound transducer is essential to ensure high-quality images and accurate diagnoses. To do so, several aspects need to be considered:
Frequency
One of the key factors in the choice of transducer is the frequency, which is responsible for measuring the relationship between penetration depth and image resolution.. This is an essential aspect, as it determines its ability to penetrate the tissues and provide a clear image.
High frequency (greater than 7 MHz)
- Offers more detailed imagesbut with less penetration capacity.
- It is the ideal frequency for surface structures such as muscles, blood vessels and skin.
- Used in linear and endocavity transducers.
Low frequency (less than 5 MHz)
- Allows a increased penetration. However, its resolution is lower.
- It is used to evaluate deep organs such as the liver, kidneys and heart.
- It is located in convex and sector transducers.
If the objective is to study tissues close to the surface, as in a muscle ultrasound, a high-frequency transducer is recommended. On the other hand, to explore internal organs or structures located in deep areas, a low-frequency transducer should be chosen.
2. Specific clinical application
Before choosing a transducer, the following should be done take into account the medical specialty and the type of structures to be examined What types of transducers are recommended depending on the medical application?
Vascular and musculoskeletal ultrasound
It is recommended to use a linear transducerThe high-frequency imaging allows visualization of superficial structures such as arteries, veins, muscles and tendons in great detail.
Abdominal and obstetric examinations
Use a convex transducer to achieve greater penetration. It has a low frequency that allows deep penetration to evaluate organs such as the liver, kidneys and uterus.
Cardiac and pulmonary evaluation
Select a sector transducer (phased array). It can image the heart through confined spaces such as ribs and allows real-time dynamic studies to be developed.
Gynecology and urology
Choose a endocavitary transducer with high resolution. Its high frequency allows obtaining clear images of reproductive organs such as the uterus, ovaries and prostate.
Pediatrics and neonates
A microconvex transducer provides the best resolution to size ratio. Its smaller size facilitates scanning in infants and neonates.
Ultrasound in emergency and intensive care
You need a sector or microconvex transducer because of its portability and penetration capability for rapid imaging of critically ill patients.
Advanced 3D and 4D studies
It requires a volumetric transducer with three-dimensional reconstruction.
3. Necessary field of vision
The transducer design influences the coverage area of the ultrasound image. Depending on the size of the required field of view, the following options should be considered:
- For small and detailed structuresLinear or microconvex transducers are the best choice, as they provide high-resolution images in small areas such as blood vessels, muscles and joints.
- For studies of deep organs and large structuresIn this case, convex or sectorial transducers are recommended, since they allow visualization of large areas with good penetration. For this reason, they are the ones used in abdominal and cardiac studies.
4. Mobility and ease of use
In some clinical settings, portability and transducer size are other essential factors in obtaining a more efficient diagnosis.
- Studies in the operating room or emergency roomSectorial transducers are recommended, since their compact design and penetration capacity allow ultrasound scans to be performed in small spaces.
- General inquiriesConvex and linear transducers are the most commonly used due to their ease of use and versatility.
- Ultrasound-guided procedures (punctures, biopsies)Transducers with puncture guides are preferred to improve the accuracy of needle insertion.
| Transducer Type |
Frequency (MHz) |
Penetration Depth |
Resolution |
Main Applications |
| Linear |
5 – 15 |
Download |
High |
Vascular, muscle, skin |
| Convex |
2 – 6 |
Media |
Media |
Abdomen, obstetrics |
| Sectorial |
2 – 4 |
High |
Media |
Cardiac, pulmonary |
| Endocavitary |
5 – 9 |
Download |
High |
Gynecological, prostate |
| Microconvex |
5 – 8 |
Media |
Media |
Pediatrics, anesthesia |
| 3D/4D |
Variable |
Variable |
High |
Obstetrics, cardiology |
Conclusion
The choice of transducer in ultrasound depends on the anatomical region to be evaluated and the level of detail required. From linear transducers for superficial structures to sectorial transducers for cardiac studies, each type of ultrasound probe has a specific function to optimize ultrasound diagnosis in various medical specialties.
Do you need more information? Contact us and the 4D Médica team will help you find the model that best suits the different needs of your clinic or medical center.
Contact 4D
Bibliography
Díaz-Rodríguez, N., Garrido-Chamorro, R. P., & Castellano-Alarcón, J. (2007).. Methodology and techniques.
Ultrasound: physical principles, ultrasound scanners and ultrasound language. Family Medicine. SEMERGEN, 33(7), 362-369. Retrieved from
https://www.elsevier.es/es-revista-medicina-familia-semergen-40-articulo-metodologia-tecnicas-ecografia-principios-fisicos-13109445
Borrego, R., & González Cortés, R. (2018).. Basic fundamentals of ultrasound. Spanish Society of Pediatric Intensive Care. Retrieved from https://secip.com/images/uploads/2018/09/1-FUNDAMENTOS-BASICOS-DE-ECOGRAF%C3%8DA.pdf
Pardell Peña, X. (2024). Ultrasonography and ultrasound. Authorea. Retrieved from https://www.authorea.com/doi/full/10.22541/au.172660489.98960333
DiagXimag(n.d.). Ultrasound and fluoroscopy specialists. Retrieved from https://diagximag.com/
Luis Daniel Fernandez Perez
Director of Diagximag. Distributor of medical imaging equipment and solutions.


por Luis Daniel Fernádez | Feb 28, 2025 | Equipment analysis
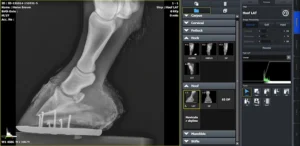
The model VIVIX-S 2530VW from the manufacturer Vieworks is a wireless flat panel detector for general radiography specifically designed for veterinary applications. It offers advanced technology with wireless connectivity and a lightweight, rugged and portable design with integrated handles, making it easy to carry and portable. Therefore, it stands out for being an indispensable tool in the area of diagnostic imaging to generate X-ray images with high precision and sharpness in small and large animals.
What are its main technical features, advantages and clinical applications? The following is an analysis of the equipment, detailing each of these aspects.
Technical characteristics of the VIVIX-S detector for veterinary use
This detector digital radiology The latest generation of combination of high-resolution technologya compact and portable design and a high resistance. At the same time, it is a multipurpose medical equipment that can be used in different environments, both in veterinary hospitals and in mobile clinics. Specifically, it has the following technical features:
Superior image quality
Thanks to its high Modulation Transfer Frequency Frequency (MTF) and Detection Quantum Efficiency (DQE), this detector provides accurate diagnostics and some images of X-rays with great clarity. With a pixel size of 124, the anatomical details of internal organs and tissues are visualized with a high definition. Therefore, it is a medical team that plays a key role in the evaluation of fractures, soft tissues and bone structures in animals.
Portable and lightweight design
The VIVIX-S 2530VW panel is easy to use and handleas it has a size 25.4 cm x 31.7 cm (11.5 in. x 11.5 in.) and a weight of 1.95 kg (including the battery). But, in addition to its ergonomic and lightweight design, it incorporates some handles for easy carryingadding convenience and comfort. This makes it a medical equipment ideal for all types of professionals, both those working in veterinary clinics and in field environments.

Strength and durability
It is designed to withstand harsh conditions and is equipped with the IP67 certificationwhich means that it is resistant to both dust and water. In addition, it offers a large temperature stabilityfrom 0 to 40 degrees Celsius.
To check your resistance and durabilityIt has been tested against drops of up to 1 meter and can withstand loads of up to 400 kg. Thus, it differentiates itself as a device that can be used in the veterinary diagnosis of large animals.
Long battery life and versatile charging
The 3400 mAh lithium-ion battery allows up to 1,250 exposures in a 15-second cycle and an autonomy of 8 hours in standby mode. In addition, it offers multiple loading optionsUSB-C connection, charging cradle and an innovative magnetic charging system, guaranteeing a continuous operation without interruption.
Advanced connectivity
It is equipped with Wi-Fi connectivity (802.11n/ac) and Gigabit Ethernet, so that the panel facilitates the fast image transmission without the need for cablesstreamlining the workflow in veterinary clinics. In addition, its integrated OLED display provides real-time information on battery and connection status.
Advantages of the VIVIX-S 2530VW panel
This flat panel offers multiple benefits for the veterinary medical team, optimizing the imaging process and improving diagnostic accuracy.
- Portability and ease of useThe lightweight design and the option of wireless connectivity allow it to be used in a variety of locations, from clinics to farms to animal rescue centers. For this reason, it is an equipment that can be used in veterinary examinations in different environments.
- High image qualityIts advanced image processing, using PureImpact™ technology, enhances image quality in contrast and sharpness. PureImpact™ is a post-processing algorithm that incorporates fine details without visual artifacts, such as soft tissue delineation, grid-free chest processing and clear, sharp resolution.
- Durability and resistanceRobust construction ensures reliable performance and increased durability, even under adverse conditions. For this reason, this device becomes a good long-term investment.
- Optimization of working timeRapid image capture and transmission reduces consultation waiting times, which translates into a better veterinary experience and care.
VIVIX-S integration with VXvue image acquisition software
On the other hand, it also includes integration with VXvuea digital radiographic image acquisition software specifically designed for the detectors of the Vieworks VIVIX-S series. This software offers a comprehensive solution for the acquisition and management of radiographic images, maximizing efficiency and accuracy in medical and veterinary environments. Its main functionalities are detailed below:
DICOM 3.0 compatibility
The DICOM medical image communication standard ensures efficient integration and communication with other medical imaging systems, facilitating data storage and transfer. It is responsible for the definition of the file format and structure and, at the same time, establishes a communications protocol to facilitate a proper connection between different medical equipment, devices and systems.
Integration with QXLink PACS system
At the same time, it can also be connected with the Vieworks QXLink PACS systemallowing for a centralized and secure management of medical imaging and patient data. Using a PACS systemdiagnostic images can be accessed anytime and anywhere via the Internet. It is therefore a key tool in medical diagnostics, as it offers great flexibility in the visualization of studies.
Advanced image processing with PureImpact™.
The PureImpact™ postprocessing algorithm provides a advanced image processing, increasing quality and resolution of radiographs. It excels in generating fine details without visual artifacts, accurate soft tissue delineation and elimination of grid lines, even in non-grid chest X-rays.
Automated functions
Includes tools such as image auto-assembly, automatic cropping, and automatic labelingThe new system is designed to streamline the image acquisition process and improve your operational efficiency.
Multi-task patient management
Allows you to manage multiple patients simultaneouslyThis facilitates the acquisition of images of different individuals in parallel.
Multilingual interface
The software is available in several languagesincluding English, Spanish, French, Italian, German, Russian, Chinese and Japanese, and offers the possibility of adding other languages according to the user's needs.
Optimized touch interface
This software is designed for your use on tablets and touchscreens. In addition, it features larger icons and fonts for intuitive operation, as well as specialized functions. These include gripper zoom and tactile scrolling.
Easy customization
Offers three types of image processing (soft, normal and hard) to suit the individual preferences of veterinary professionals. It also allows customization of themes and layouts, including automatic interface rotation for vertical monitors.
Optimization for various applications
The VXvue software is configured for its use in general human and veterinary radiography (with specific options for dogs, cats, exotic animals and equines) and mobile X-ray systems. Therefore, it is a software that adapts to the specific needs of each clinical environment.
Clinical uses and applications
The VIVIX-S 2530VW detector is a very versatile tool that adapts to various specialties within veterinary medicine. Some of its main applications include:
- Diagnostic imaging in small and large animalsHigh-resolution radiographs can be obtained to evaluate fractures, joint injuries, lung disease and internal organ abnormalities.
- Surgical proceduresIts ability to generate high-precision images in real time facilitates the work of veterinarians during orthopedic surgeries and invasive procedures.
- Dental examinationsThe detailed resolution of the panel is ideal for evaluating caries, infections and structural anomalies in the dentition of dogs, cats and horses.
- Orthopedic and neurological evaluationsIt is especially useful for detecting dysplasias, spinal conditions, joint problems and neurological lesions.
Conclusion
VIVIX-S 2530VW is a wireless detector for general radiography in veterinary medicine that has a high durability, portability and image quality. Its technology and innovation not only facilitates fast and accurate diagnosis, but also improves your efficiency in the clinical setting and veterinary practice.
At 4D Médica, we have this medical equipment specialized in the veterinary area.. If you are looking for a complete digital radiography solution that can be adapted to different uses, this flat panel is one of the best options on the market.
Do you need more information? Contact us and we will offer you personalized advice according to your needs.
Contact 4D
Luis Daniel Fernandez Perez
Director of Diagximag. Distributor of medical imaging equipment and solutions.

por Luis Daniel Fernádez | Feb 14, 2025 | Equipment analysis
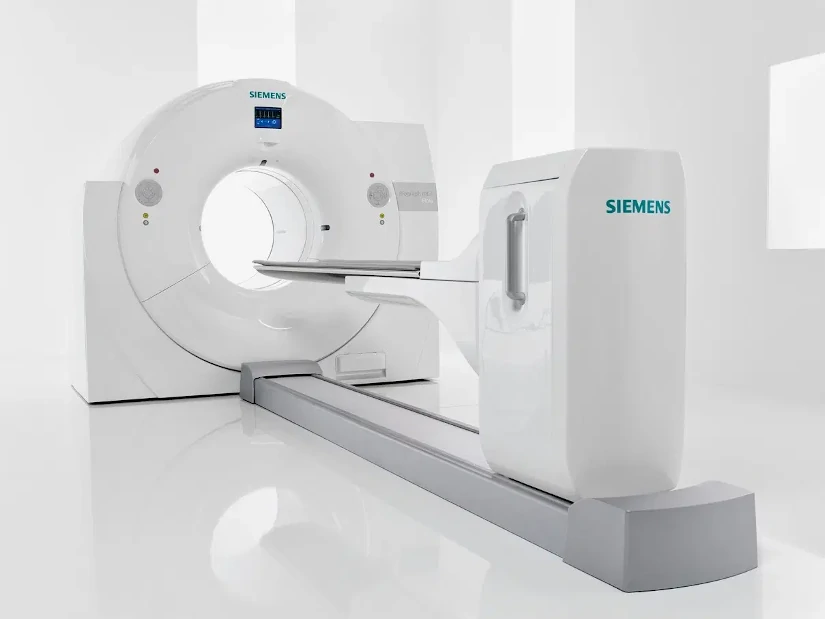
The PET technique CT consists of the integration of two imaging technologies in the same medical equipment: Positron Emission Tomography (PET) and Computed Axial Tomography (CT). The first PET-CT prototype was developed at the University of Pittsburgh in 1998 and its commercialization began in 2001, making it one of the first PET-CT scanners in the world. the most innovative and up-to-date equipment of the area of diagnostic imaging.
A PET CT system is a hybrid medical equipment with a stretcher and a shared medical image acquisition systemThe combination of both technologies provides a tomographic image that represents a cross-section of the organism, offering anatomical and functional information of the interior of the human body. The combination of both technologies provides a tomographic image that represents a cross section of the organism, offering anatomical and functional information of the interior of the human body.
On the one hand, the technology of Positron Emission Tomography or PET scanning provides functional and molecular information of the tissues through the use of a radiopharmaceutical. Therefore, it allows the quantification of various biochemical processes. From cellular metabolism, blood flow and protein synthesis to the analysis of different receptors. For its part, the Computed Axial Tomography or CT reports the different tissue densities generating a high-resolution anatomical image.
Thus, by combining the two techniques in a single integrated PET CT systemcan be generated anatomical and functional images simultaneously. As a result, more complete and efficient clinical diagnoses are offered, both in terms of sensitivity and specificity. Through its ability to detect functional alterations before they are visible in conventional studies, PET CT is fundamental in the early detection of diseases and in the evaluation of the effectiveness of treatments. Especially in enceological, neurological and cardiac diseases. In the following article, we analyze how it works and its main uses in clinical practice.
How does the hybrid PET CT equipment work?
The medical image acquisition protocol in a PET CT study is similar to the procedure for the standard PET technique. In a PET CT scanner, the acquisition of the study consists of three phases: the performance of a topogram, the performance of a CT study that will make it possible to determine the attenuation correction of the PET technique and, finally, the acquisition of the Positron Emission Tomography (PET). Each of these phases is discussed below:
Patient preparation
Before performing a PET CT study, the patient must be properly prepared so that the medical images obtained are of optimum quality. First of all, a radiopharmaceutical is administeredThe most widely used is Fluorine-18-labeled Fluorodeoxyglucose (18F-FDG). This compound makes it possible to detect areas of high metabolic activity that often arise in certain types of cancer, neurological and cardiac diseases. The radiopharmaceutical is administered intravenously and the patient must wait between 45 and 60 minutes for it to distribute correctly by the agency prior to the start of image acquisition.
For optimal uptake of the radiopharmaceutical, the patient must follow a series of medical recommendations:
- Fasting for at least 4-6 hours before the study.which avoids interference with glucose metabolism.
- Staying well hydrated before and after of the procedure.
- Control blood glucose levelsThe high levels may affect the uptake of the radiopharmaceutical.
- Follow instructions from physical rest before the study. Excessive movement prior to the study may generate unwanted FDG accumulation in the muscles.
- In some cases, a controlled breathing protocol to improve the quality of the CT image.
2. Positioning of the patient in the tomograph
Once the waiting period after injection of the radiopharmaceutical is over, the patient is placed on the bed of the PET CT scanner.. To obtain high quality images and reduce errors in PET and CT image superimposition, it is essential that the patient is well aligned and comfortable. In turn, The patient is asked to extend the arms over the head. if possible, to reduce interference in the images of the thorax and abdomen. On the other hand, metal objects are removed and elements that may affect image quality.
Subsequently, the position of the stretcher is adjusted according to the area to be examined, ensuring that the body is well aligned with the CT scanner detectors. In this process, patient immobility is crucial to avoid blurred images and improve diagnostic accuracy.
3. Making the topogram
The first step in the examination of the patient is to perform a topogram with the PET CT equipment. The images are obtained using the X-rays in a fixed position, which can be anterior, posterior, lateral or in an intermediate orientation. The acquisition is performed with a continuous movement of the stretcher in a predetermined range. In this way, a anatomical image similar to an X-ray projectionwhere the different internal structures and tissues can be analyzed.
It is important that during the procedure the equipment is adjusted and the limits of the PET CT study are defined. Depending on the model of the CT scanner, the fields of view and image formation may be different for different techniques. Therefore, it is necessary to verify that all body parts are within the image with the smallest field of viewwhich are normally those of the CT scan.
4. Elaboration of the TAC study
Once the field of view of the PET CT study has been defined, the patient's stretcher is automatically mobilized to start the CT diagnosis. In the test, a specific breathing protocol is introduced to match the CT and PET image, since the latter is acquired with normal breathing by the patient.
The duration of the CT study depends on various parameters: the extension of the area to be scanned, the rotation speed of the tube and the translation of the stretcher. CT allows detailed anatomical images to be obtained through the use of X-rays, which facilitates the precise localization of organs and structures. In some cases, a contrast medium may be administered to enhance the visualization of vascular structures or specific lesions.
Regarding its duration, a full body CT study using the hybrid equipment is less than one minute. This is because the images obtained are used for attenuation correction in the PET study, which significantly reduces the acquisition time. In PET equipment, when germanium (Ge) sources are used, the CT procedure time amounts to 20 to 30 minutes. With this, radiation exposure is reduced and the patient experience is improved.
5. Acquisition of the PET study
After the CT analysis, PET images are acquired, in which the metabolic data of the tissues are captured. For this purpose, the couch is moved to position the patient in the field of view of the PET scanner, encompassing different positions on the stretcher to cover the region of interest to be analyzed. All these areas are the ones that cover the range explored by CT.
The acquisition time of the PET study can range from between 10 and 30 minutes. This depends on the stretcher positions, the range scanned, as well as the equipment used. During this phase, the areas of the body with abnormal metabolic activity are highlighted on the PET imageThis makes it possible to detect tumors, infections or neurological problems with great precision.
6. PET CT image reconstruction
Reconstruction is performed in parallel to image acquisition.This allows results to be obtained in just a few minutes. This step is essential to generate highly accurate fused images, combining the metabolic information from PET with the detailed anatomical structure from CT.
In this process, the reconstruction time of each CT slice is less than one second.The PET images are reconstructed and available for analysis at the end of the acquisition of the last couch position. To achieve this, we use the reconstruction algorithms available in PET tomographs with the scatter and attenuation corrections determined from CT images.
7. Image analysis and interpretation
Once the images have been reconstructed, they are analyzed, where specialists can analyze different types of medical images:
- PET images without correctionThey show the uptake of the radiopharmaceutical in the body.
- Corrected PET imagesThey incorporate attenuation adjustments to improve accuracy.
- CT imagesThey offer anatomical details of the explored region.
The image fusion software allows the superimposition of PET and CT information, facilitating the exact localization of lesions and their subsequent analysis and interpretation.
What is PET CT used for?
It is a diagnostic technique that is essential in different medical specialties:
- OncologyEarly detection of tumors, evaluation of metastases and treatment follow-up.
- NeurologyIt is used for the diagnosis of diseases such as Alzheimer's, Parkinson's and epilepsy.
- CardiologyThey play an essential role in the evaluation of blood flow and the detection of lesions and abnormalities in the heart.
- Immunology and infectionsHelps in the identification of inflammatory processes and infectious diseases.
Source || Canva
Clinical applications of PET CT
PET CT technology combines the advantages of an anatomical and a functional imaging technique. In the current medical context, the use of this hybrid equipment is used in the following cases:
To confirm or rule out a malignant tumor pathology.
The PET technique can to analyze whether a lesion is benign or malignantThis can avoid the need for biopsies and other invasive diagnostic tests. In turn, it allows early detection of tumor processes, before anatomical changes occur that can be detected by morphological imaging techniques.
Determine tumor extent
It has the ability to perform whole body studieswhich makes it possible to rule out or confirm other malignant lesions concurrent with the primary tumor.
Detecting new tumor recurrences
Through this technique, it is possible to differentiate between malignant processes and new tumors that arise recurrently. This can be used to optimize patient treatment planning.
Assess response to treatment
The metabolic changes produced before an adequate response to chemotherapy are observed earlier in PET imaging than in other techniques. diagnostic imaging. Therefore, this type of medical imaging is an early indicator of tumor response. Their use helps to determine the continuation of certain treatments or, on the contrary, their interruption.
Conclusion
The use of hybrid PET-CT equipment is a crucial advance in medical diagnostics. It combines a functional and anatomical analysis of the inside of the human body in a single medical device, making it fundamental in the early diagnosis of cancer and other neurological and cardiological diseases. The combination of technology and medicine continues to save lives, and the PET CT technique is a clear example of this.
If you want to get information about PET-CT or other radiodiagnostic equipment, you can contact us. Our 4D team will give you advice to find the best solution for your clinic or hospital.
Contact 4D
Bibliography
Instituto de Salud Carlos III (n.d.).
PET/CT Image Acquisition and Processing Handbook. REPISALUD. Retrieved February 13, 2025, from
https://repisalud.isciii.es/rest/api/core/bitstreams/5a1cd1bb-f736-4746-aa8c-0cc3a0a7a274/content
Medigraphic (2005). Acta Médica Article. Retrieved February 13, 2025, from https://www.medigraphic.com/pdfs/actmed/am-2005/am053e.pdf
Electronic Journal of University Medical Science (n.d.). Article in RECIAMUC. Retrieved February 13, 2025, from https://www.reciamuc.com/index.php/RECIAMUC/article/view/1326/2074
Medigraphic (2014). Acta Médica Article. Retrieved February 13, 2025, from https://www.medigraphic.com/pdfs/actamedica/acm-2014/acm141i.pdf
Martínez del Valle, M. (2016). PET-CT: Physical basis, instrumentation and technological advances. Radiology, 58(5), 377-389. Elsevier. Retrieved from https://www.elsevier.es/es-revista-radiologia-119-articulo-pet-tac-bases-fisicas-instrumentacion-avances-S0033833816301801?newsletter=true
Spanish Society of Nuclear Medicine and Molecular Imaging (SEMNIM). (2019). PET-CT protocol. SEMNIM. Retrieved February 13, 2025, from https://www.semnim.es/wp-content/uploads/2019/07/79.pdf
Luis Daniel Fernandez Perez
Director of Diagximag. Distributor of medical imaging equipment and solutions.

por Luis Daniel Fernádez | Jan 31, 2025 | Equipment analysis
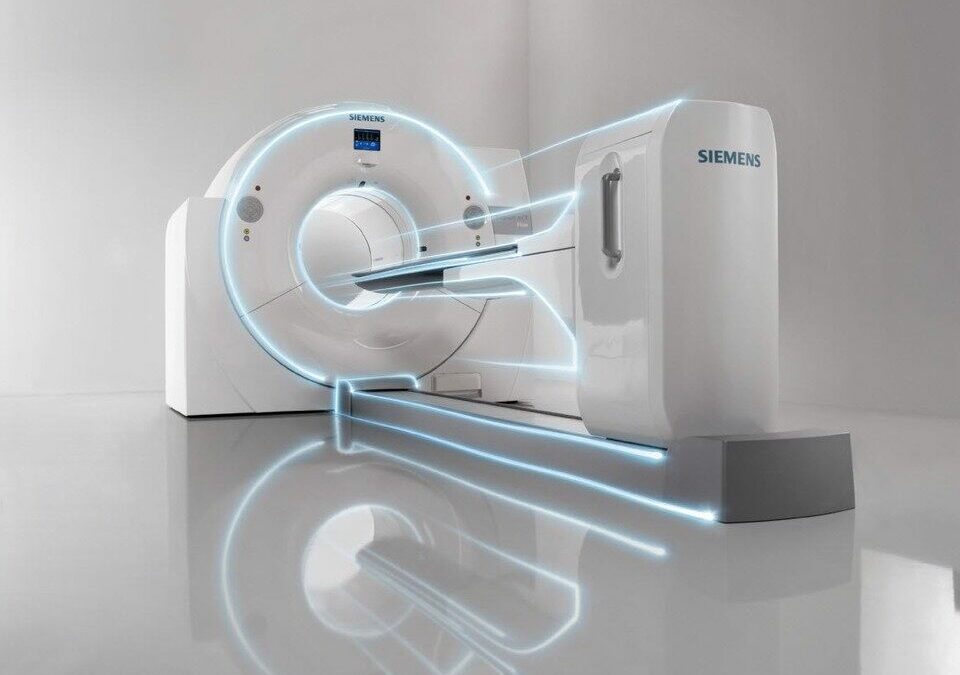
The positron emission tomography (PET) scanning is the technique of diagnostic imaging more recent and modern. It is a nuclear medicine procedure that emerged in the 1970s in the United States and was introduced in Spain in 1995. To perform a positron emission tomography scan, a radioactive material, called a radiopharmaceutical, is administered intravenously and the diagnosis is then made using specific equipment: the PET scanner.
This medical device is equipped with a special camera that allows visualization of internal organs at the molecular and cellular leveloffering information on metabolic activity of the body's tissues. From the analysis of blood flow, oxygen consumption, glucose and protein metabolism, amino acid transport and cell division to the detection of biochemical changes.
In the PET technique, radioation is detected after administration of the radiopharmaceutical. To do this, you need a waiting time between 30 and 60 minutes for the substance to take effect and be distributed correctly throughout the patient's body. This diagnostic imaging test is used for to develop a metabolic study of the interior of the organismIt therefore provides a complement to the anatomical information offered by procedures such as computed tomography (CT) or magnetic resonance imaging (MRI).
One of the most recent advances in this area has been the development of hybrid equipment that combines two technologies in the same medical equipment. In 1998, the CT scanner began to be used in clinical practice. PET CTa device that incorporates the PET technique together with CT. A year earlier, in 1997, the hybrid PET MRI device was created by Mardsen and Cherry, which combines the anatomical images provided by MRI with the biochemical data from PET. However, it was not until 2009 that Phillips developed the first integrated system.
Currently, the use of positron emission tomography (PET) has made it possible to diagnose diseases in their earliest stages and, in turn, analyze the patient's response to specific treatments. Its ability to analyze functional changes before structural damage occurs in the body makes it key in the diagnosis and monitoring of multiple pathologies, especially in oncology, neurology and cardiology.
In the following article, we will analyze what this diagnostic technique consists of and the medical equipmentThe advantages and disadvantages, as well as their applications in clinical practice.
How does PET positron emission tomography work?
The positron emission tomography diagnosis consists of a process made up of different stages, which we analyze below:
Administration of the radiopharmaceutical
The first step in a PET study is the administration of a radioactive substancecalled radiopharmaceutical or radiotracer. This compound is generally introduced into the body intravenously, although in some cases it can be administered by inhalation or orally.
The most commonly used PET radiopharmaceutical is fluorodeoxyglucose (FDG). It consists of a glucose-like molecule that is labeled with fluorine-18, a radioactive isotope. The main reason for using FDG is that cells with high metabolic activity, such as cancer cells, consume more glucose than normal tissues. This allows the radiopharmaceutical to accumulate in areas of higher cellular metabolism, facilitating its detection.
2. Distribution and waiting
After administration of the radiopharmaceutical, the patient must remain at rest for 30 to 60 minutes for the substance to be adequately distributed throughout the body. During this time, it is recommended that the patient remain calm and avoid talking or moving excessively, since muscular activity could alter the uptake of the radiotracer and affect the quality of the images.
3. Patient positioning
Once the radiopharmaceutical has been absorbed by the tissues, the patient is placed on a sliding stretcher which introduces it into the PET scanner.. This equipment consists of a ring of detectors that surrounds the patient and is capable of recording the radiation emitted by the radiopharmaceutical. The procedure has a duration between 15 and 45 minutesdepending on the type of study to be performed.
4. Diagnosis by PET scanner
The radiopharmaceutical injected into the patient emits positrons.which collide with the body's electrons, generating two gamma photons in opposite directions. The PET scanner detectors capture these gamma photons and record the exact location of each emission. Subsequently, the medical team is responsible for the reconstruction of a tomographic image detailed with the areas where the radiopharmaceutical has accumulated, reflecting the metabolic activity of tissues and organs.
5. Image processing and reconstruction
Once the data has been collected, specialized software processes the information and generates three-dimensional images of the distribution of the radiopharmaceutical in the patient's body. These images show the areas of increased metabolic activity (hyper uptake) in brighter colorswhile areas with lower metabolism appear in darker shades. This activity map allows physicians to accurately identify anomalies such as malignant tumors, neurodegenerative diseases or cardiac conditions.
6. Analysis and interpretation of results
Finally, specialists in radiology or nuclear medicine analyze the images. obtained to make a diagnosis. Depending on the case, the PET scan can be combined with other imaging techniquesas the computed tomography (CT) or the magnetic resonance imaging (MRI)as well as the use of hybrid equipment. This will provide a more complete view of the anatomy and function of the organs.
Source || Canva
Positron emission tomography advantages
Positron emission tomography (PET) is a highly advanced imaging technique with the following benefits:
Early detection of diseases
Allows you to identify metabolic abnormalities before visible structural changes occur in other imaging tests, which facilitates the early diagnosis of diseases. These include cancer, Alzheimer's disease and heart disease.
Real-time functional evaluation
In contrast to computed tomography (CT) or magnetic resonance imaging (MRI), which only analyze anatomy, PET provides information on how tissues and organs function at the cellular and molecular level.
Effective technique to detect cancer and metastases
PET is one of the most effective tools for the detection and localization of cancer and its metastasesThis allows us to know the extent of the disease and to plan the appropriate treatment.
Monitoring treatment response
This is a diagnostic technique used for evaluate how a patient is responding to chemotherapy, radiotherapy or immunotherapy treatments. In this way, it makes it possible to make adjustments to the therapeutic strategy in real time.
Combined technology for greater precision
The use of hybrid equipment allow both anatomical and functional information to be obtained at the same time. At present, PET-CT and PET-MRI equipment offer the most advanced benefits of using two techniques in a single study. Its use helps to improve diagnostic accuracy and radiation dose reduction received by the patient by up to 50 %.
Disadvantages of positron emission tomography
However, it also has a number of limitations that are important to analyze:
Exposure to ionizing radiation
The PET technique uses radioactive radiopharmaceuticals that expose the patient to ionizing radiation. Although its doses are low and safe, the amount of radiation increases significantly when using various diagnostic techniques.
High cost and limited availability
It is a expensive technique because of the need for specialized equipment and the use of radiopharmaceuticals. These substances require rapid distribution in order not to lose effectiveness. Therefore, one of their disadvantages is that they limit availability in certain hospitals and regions.
Waiting time and duration of the study
Before performing the PET scan, patient must wait 30 to 60 minutes after injection of the radiopharmaceutical. Thus, in comparison with other diagnostic techniques, waiting time increases the duration of the test.
Complex interpretation of images
Medical images obtained can be difficult to interpret.not all elevated glucose uptake indicates abnormalities. Therefore, alternative tests are required for a more accurate diagnosis.
Clinical uses and applications
Positron emission tomography is used in different medical specialties, specifically in oncology, neurology and cardiology. What are its main uses in clinical practice?
Oncology
- Early detection of malignant tumors.
- Identification of metastases and evaluation of cancer spread.
- Assessment of the response to treatment with chemotherapy or radiotherapy.
- Differentiation between benign and malignant tumors.
Neurology
- Early diagnosis of neurodegenerative diseases such as Alzheimer and Parkinson.
- Localization of epileptic foci in patients with treatment-resistant epilepsy.
- Evaluation of psychiatric illnesses and neurocognitive disorders.
Cardiology
- Determination of cardiac muscle viability in patients with myocardial infarction.
- Evaluation of blood flow and cardiac function in ischemic diseases.
Other medical applications
- Diagnosis of endocrine diseases, such as adrenal gland disorders.
- Detection of infections and chronic inflammatory diseases.
- Evaluation of gastrointestinal pathologies with metabolic involvement.
Conclusion
After analyzing the operation of positron emission tomography (PET), we can highlight that it is a fundamental tool in nuclear medicine to detect diseases in their early stages and evaluate the metabolic function of different organs and tissues.
Do you want more information about PET equipment? Contact us and we will offer you personalized advice to analyze the medical equipment you need in your clinic or hospital.
Contact 4D
Luis Daniel Fernandez Perez
Director of Diagximag. Distributor of medical imaging equipment and solutions.

por Kiko Ramos | Jan 17, 2025 | Equipment analysis
The radioprotection is the set of measures, standards and practices aimed at protecting people, the environment and the surroundings from the harmful effects of ionizing radiation. In the clinical setting, the aim of radiation protection is to ensuring the safe use of radiation for diagnostic and therapeutic procedures for patients and healthcare personnel, minimizing the associated risks.
What is radioprotection?
The ionizing radiation is a fundamental tool in modern medicine. It is used in procedures of diagnostic imaging that use X-rays, such as conventional radiography, digital radiology, fluoroscopy, computed tomography (CT) and interventional radiologyRadiology, a branch of radiology that diagnoses and treats various pathologies by means of minimally invasive procedures. In turn, it is also used in radiotherapy treatmentsThe aim of this program is the destruction of tumor cells and tissues by means of radiation, and in the nuclear medicine.
However, its improper or excessive use can have harmful consequences for people's health.. These include tissue damage or increased risk of cancer in the long term. For this reason, it is of great importance in the clinical environment and requires a sound management. In this sense, the discipline of Radiation ProtectionThe company, which employs professionals such as physicists, physicians, biologists and engineers, is working to ensure that the development and application of technologies that use ionizing radiation are safe.
Basic principles of radiation protection
The Radiation Protection System is based on three fundamental principles that have been established by the International Commission on Radiological Protection (ICRP):
1. Justification
Any procedure involving the use of ionizing radiation must be medically indicated. This means that the benefits of the procedure must clearly outweigh the risks associated with radiological exposure.
2. Optimization (ALARA Principle)
Exposure should be kept "as low as reasonably achievable". This principle is referred to as ALARA and ensures that the lowest dose necessary to obtain clinical results is used.
3. Dose limitation
Strict dose limits must be established to protect both healthcare personnel and patients, preventing exposure from exceeding levels considered safe. This principle is oriented to the protection of persons exposed to radiation sources.
Application of the Radiological Protection System in the clinical environment.
In the clinical environment, the Radiation Protection System is implemented through a structured approach that includes the following aspects:
Design and maintenance of installations
The rooms of X-raysCT scans, CT scans or TAC and radiotherapy must be equipped with adequate shielding that minimizes radiation scattering. In turn, it is essential to carry out periodic inspections to guarantee the correct functioning of medical equipment and that they do not emit an unnecessary dose of radiation.
Equipment quality control
The following must be implemented preventive maintenance and calibration programs to ensure that the equipment operates efficiently within the established limits. Another key aspect is incorporate advanced technologies that allow automatic adjustment of radiation doses according to the patient's characteristics. To this end, digital radiology medical equipment will make it possible to optimize the amount of radiation, increasing safety in the healthcare environment for both medical staff and patients.
Staff training
One of the strategies to promote radioprotection in the clinical setting is to to train health professionals on the safe use of medical equipment that emit ionizing waves and which, in turn, have knowledge of the three principles of radioprotection. In this way, through appropriate training, it will be possible to promote the development of a safety culture to ensure the application of good practices in daily work in the health sector.
Radiation protection measures
Radiation protection in the clinical environment is essential to ensure the safety of patients and healthcare personnel from the risks associated with ionizing radiation. To this end, various strategies and tools designed to minimize unnecessary exposure are implemented, respecting the principles of justification, optimization and dose limitation.
Protection of healthcare personnel
Personnel working in areas where ionizing radiation is used must be adequately protected to avoid cumulative exposure that may pose a long-term risk. Key measures include:
- Personal Protective Equipment (PPE)Professionals should wear leaded aprons, thyroid protectors, leaded goggles and gloves that are specifically designed to reduce direct exposure to radiation.
- Dose monitoringIt is mandatory for health personnel to record the amount of radiation accumulated. This monitoring ensures that the dose does not exceed the limits established by the regulations in force.
- Staff turnoverTo minimize exposure time, personnel rotation is organized in tasks involving the handling of radiation-emitting equipment. In this way, the exposure load is evenly distributed.
Get to know our 4D Médica protection equipment
Patient protection
Patients should also be protected from unnecessary radiation exposure, especially considering that they are often exposed in a timely manner but with high doses in some diagnostic or therapeutic procedures. The most relevant measures are:
- CollimationIt is essential to limit the area of the body that is exposed to radiation by using collimation systems that focus the radiation beam only on the area of interest. This reduces the amount of tissue irradiated and thus the associated risks.
- Optimized protocolsModern equipment makes it possible to adjust the exposure parameters (such as energy and radiation time) according to the specific characteristics of each patient. This makes it possible to deliver a minimum dose without compromising the quality of the radiation dose. medical images or treatment.
- Repetition controlTo avoid unnecessary repetitions of radiological studies, it is essential that the staff is well trained and that the equipment is functioning optimally. This ensures that the images obtained are of diagnostic quality on the first attempt.
Signaling and delimitation of areas
Facilities using ionizing radiation must have proper signage and access control to protect those not involved in the procedures. These measures include:
- SignageVisible signs should be posted indicating radiological risk areas and exposure levels, warning people of the need to wear appropriate protection or to avoid entry.
- Delimitation of areasIonizing radiation: Access to areas where ionizing radiation is used should be restricted. Its use should be limited to authorized personnel, thus avoiding accidental exposure of third parties or the general public.
Conclusion
The radioprotection in the clinical environment is a shared responsibility that requires the collaboration of professionals, patients and regulatory bodies. Applying protection principles and measures not only ensures safety, but also improves the quality of medical care.
If you want to get more information about protective equipment or medical diagnostic equipment, you can contact us. Our 4D team will advise you to find the best solution for your clinic or hospital.
Contact 4D
Kiko Ramos
CEO of 4D Médica. Expert in marketing and distribution of medical equipment.